Mesothelioma / Sites of Mesothelioma
Sites of Mesothelioma
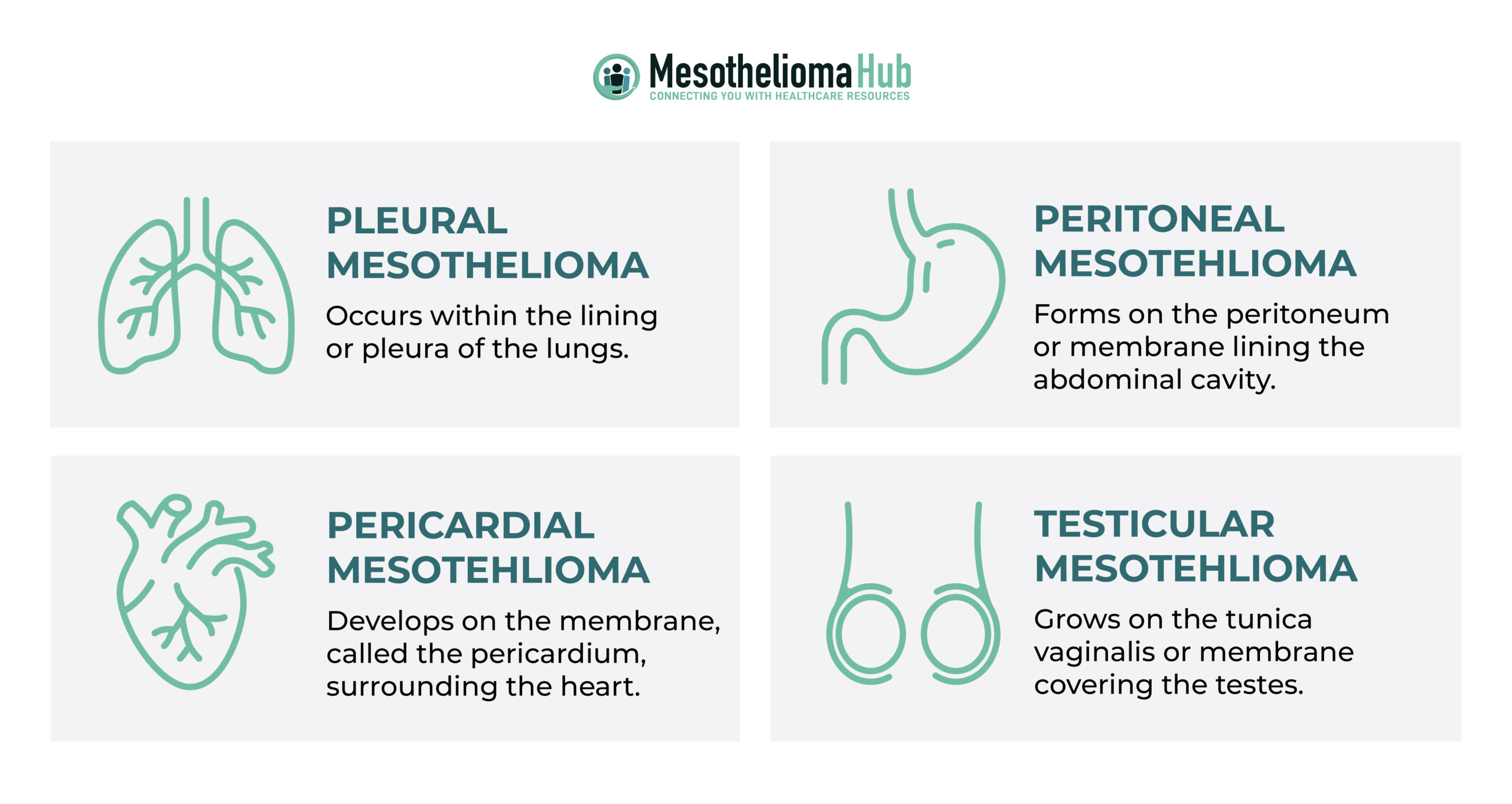
There are four locations where tumors may develop, each with its own set of symptoms and treatment plan. Pleural mesothelioma is the most common, which involves tumors growing on the tissue lining of the lungs. The following site is in the peritoneal area, or the tissue lining the abdomen. Next is mesothelioma is in the pericardium, which is the tissue lining the heart. This type occurs in less than five percent of patients diagnosed with mesothelioma. The rarest of mesothelioma is testicular.
Get Free Mesothelioma Guide
What Are the Different Sites of Mesothelioma?
This is a form of cancer that affects the mesothelium, the thin membrane of epithelial cells that lines the lungs, abdomen, and heart. There are four main sites that this cancer can develop (the pleura, peritoneum, pericardium, and the testes) from exposure to asbestos fibers. Other sites of the body can also be affected by mesothelioma tumors, like the testicles and ovaries, though it’s much less common. The type of mesothelioma depends primarily on the location, or sites, of the tumors in the body. It can also be further categorized according to the type — or types — of cancer cells present.
Both the location and cell type can significantly impact the patient’s prognosis and treatment options.
Pleural Mesothelioma
After breathing in asbestos dust, the asbestos fibers lodge in the lining of the lungs and chest. Over time, the fibers irritate the pleural lining, causing scar tissue and inflammation. Eventually, the cells can mutate and form malignant tumors. These tumors are most likely to form in the pleura (the lining around the lungs) mesothelium. When the tumors grow in this site of the body, it is called pleural mesothelioma.
This is the most prevalent type, affecting between 70 and 90 percent of patients are diagnosed with this form. Although the prognosis depends on the stage and cell type, the average life expectancy for patients with this condition is between 8 and 21 months.
Pleural Meso Symptoms
- Chest pain (35–71% of patients)
- Fatigue (18–33% of patients)
- Fever (6–33% of patients)
- Persistent dry cough (6–37% of patients)
- Shortness of breath (35–82% of patients)
- Weight loss (9–59% of patients)
The majority (54–87 percent) of patients also experience a buildup of fluid around the lungs (called pleural effusion), which can make breathing difficult and painful.
Because the symptoms mirror those of other respiratory illnesses — such as the flu, COPD, and pneumonia — as well as other types of cancer, the process to diagnose pleural mesothelioma is often a lengthy one. The diagnosis process typically includes imaging tests, blood tests, and biopsies. For pleural specifically, doctors may perform needle biopsies, such as a pleural biopsy or thoracentesis; camera-assisted biopsies, such as a thoracoscopy or mediastinoscopy; or a surgical biopsy called a thoracotomy when other biopsies fail to provide definitive results.
Treatment options depend on the stage but generally involve a combination of treatments — referred to as a multimodal treatment plan — including:
- Surgery
- Chemotherapy
- Radiation
- Immunotherapy
The two primary surgical options for pleural mesothelioma are pleurectomy with decortication, in which the linings of the lung and chest are removed, along with any visible tumors; and extrapleural pneumonectomy, in which the entire affected lung, the pleural linings of the chest and heart, and portions of the diaphragm are removed. Other surgical procedures such as pleurodesis and thoracentesis may be used to remove fluid that has built up around the lungs to make breathing easier and less painful.
Patients often undergo chemotherapy after surgery in order to destroy any remaining cancer cells; the most common chemotherapy treatment for pleural mesothelioma is a combination of ALIMTA® (pemetrxed) and cisplatin or carboplatin. Chemotherapy may also be used in lieu of surgery as an aggressive, potentially curative treatment or as a palliative treatment to improve the quality of life for late-stage patients.
Radiation may be used before, during, or after surgery to shrink and reduce the spread of tumors in pleural mesothelioma patients. It has also been shown to be effective on its own as a palliative treatment to mitigate its symptoms by reducing chest pain and easing breathing difficulties.
Immunotherapy drugs are becoming increasingly common in the treatment of pleural mesothelioma. Immunotherapy harnesses the body’s own immune system to attack malignant cancer cells.
Peritoneal Mesothelioma
Peritoneal mesothelioma can be caused by ingesting asbestos. After swallowing asbestos dust (either through the mouth or after inhaling it into the sinuses), the asbestos fibers become lodged in the lining of the abdomen. Once there, the fibers irritate the peritoneum, causing inflammation and scar tissue. In time, the cells of this scar tissue mutate and create malignant tumors in the abdominal cavity.
Peritoneal mesothelioma is the second most prevalent form; between 10 and 30 percent of patients are diagnosed with this type of cancer. The prognosis for peritoneal is better than that of other types. Although the survival rate depends on the stage and cell type, the average life expectancy for patients is between 34 and 92 months.
Peritoneal Meso Symptoms
- Abdominal pain (27–69% of patients)
- Abdominal distension (30–80% of patients)
- Diarrhea (17% of patients)
- Fatigue (11–43% of patients)
- Fever (22% of patients)
- Hernia (7–12% of patients)
- Nausea or vomiting (11–15% of patients)
- Weight loss (32–38% of patients)
Many patients (36–90 percent) also experience a buildup of fluid in the abdomen (called ascites), which can cause additional pain and bloat.
Because the symptoms mirror those of other abdominal illnesses — such as IBS — as well as stomach or ovarian cancer, diagnosing peritoneal mesothelioma, can take weeks or even months. Diagnosis usually includes imaging tests, blood tests, and biopsies. For peritoneal mesothelioma specifically, doctors may perform needle biopsies, such as a paracentesis; camera-assisted biopsies, such as laparoscopy (also called a peritoneoscopy); and a surgical biopsy called a laparotomy when other, less invasive biopsies fail to provide definitive results.
A multimodal approach is recommended for the treatment of peritoneal mesothelioma. The specific treatment plan will depend on the stage, but typically includes surgery, chemotherapy, radiation, and immunotherapy. Radiation therapy is not commonly used to treat peritoneal mesothelioma.
The main treatment for peritoneal mesothelioma is a combination of cytoreductive surgery, in which the surgeon attempts to remove all visible peritoneal tumors from within the abdominal cavity; and Hyperthermic Intraperitoneal Chemotherapy (HIPEC), a heated chemotherapy wash that is applied to the abdominal cavity immediately following surgery in order to kill any cancer cells that may remain. Patients often undergo chemotherapy after surgery in order to destroy any remaining cancer cells; the most common chemotherapy treatment for peritoneal mesothelioma is a combination of ALIMTA® (pemetrexed) and cisplatin or carboplatin.
As with other cancers, chemotherapy and radiation can also be used as palliative treatment options to mitigate symptoms in late-stage patients for whom cytoreductive surgery and HIPEC are not options. Likewise, paracentesis may be used to remove fluid that has built up in the abdomen to reduce abdominal pain and swelling.
Pericardial Mesothelioma
Of all the sites of mesothelioma tumors can form, the pericardium is a rare cancer location, affecting less than 5 percent of patients. The exact causes of pericardial mesothelioma are still unclear, but doctors suspect that asbestos fibers enter the body through inhalation or ingestion, then reach the heart via the bloodstream or lymphatic system. At that point, they become embedded in the heart lining, creating scar tissue and, eventually, tumors along the lining of the heart sac.
Unfortunately, most cases of pericardial mesothelioma are only discovered at an advanced stage (usually by accident during surgery) or after death. Because of this, the prognosis is poor and the average life expectancy for patients is under one year.
Pericardial Symptoms
- Arrhythmia
- Chest pain
- Fatigue
- Heart murmur
- Weight loss
Patients may also experience a buildup of fluid around the heart (called pericardial effusion), which can cause increased chest pain and make breathing difficult and painful.
Because the symptoms mirror those of other cardiac illnesses — such as heart disease or inflammation of the heart muscle — it is difficult to diagnose pericardial mesothelioma. Diagnosis typically includes imaging tests, blood tests, and biopsies. For pericardial mesothelioma specifically, doctors may perform an echocardiogram, which uses sound waves to assess heart function; and pericardiocentesis, a type of needle biopsy.
As with other forms of this cancer, treatment options for pericardial mesothelioma depend on the stage at which the patient is diagnosed. If curative treatment is an option, it will usually involve a pericardiectomy, a surgery that involves the removal of some or all of the pericardium, as well as chemotherapy with cisplatin. Palliative treatments for this include pericardiocentesis (also called a pericardial tap) and percutaneous balloon pericardiotomy, both of which can help relieve pericardial effusion around the heart. During pericardiocentesis, a doctor uses a needle and catheter to remove fluid from the pericardium. Percutaneous balloon pericardiotomy is similar to pericardiocentesis, but the catheter has an inflatable balloon at the end, which the doctor repeatedly inflates to create a small hole in the pericardium, allowing them to drain more of the effusion. Chemotherapy may also be used to slow the spread of tumors in later-stage patients to mitigate symptoms such as chest pain or difficulty breathing.
Testicular Mesothelioma
Testicular mesothelioma is the rarest site of mesothelioma, with only a little over 113 reported cases. The cancer begins forming within the mesothelial lining of the testicles, known as the tunica vaginalis. The tunica vaginalis is what allows the testicles to have movement.
This type of mesothelioma typically affects men over the age of 55, with the best prognosis compared to other types. Nearly 49% of patients survive five years after their diagnosis, and 33% survive ten years.
Testicular Symptoms
- Swollen testicle
- Fluid buildup in the scrotum
- Tissue buildup in the testicle
Mesotheliomas are highly aggressive and fast-spreading cancers. Treatment options for testicular mesothelioma include removing the affected testicle or testicles if it has spread to both. Removing the affected areas allows doctors to prevent further spread of the mesothelioma to other organs or lymph nodes. After surgery, your mesothelioma specialist will administer chemotherapy and radiation therapy to help prevent the spread of the cancer.
What’s Next?
Your doctor will administer tests to determine which of the sites the mesothelioma tumors have developed in. They’ll be able to tell you what stage of cancer you’re in, as well as map out a cancer treatment plan based on which of the main sites the mesothelioma has developed, the stage of cancer, your general health, and other details.
Mesothelioma Support Team
Mesothelioma Hub is dedicated to helping you find information, support, and advice. Reach out any time!
