Pleurodesis is a surgical procedure used to treat collapsed lungs or reduce fluid buildup between the lung and chest wall lining. The procedure adheres the lung or lungs to the chest wall, making it easier to breathe and relieve pain.
Pleurodesis is a treatment option for pleural mesothelioma patients who aren’t eligible for more aggressive surgeries. This procedure can help treat pleural effusion or fluid buildup in the lungs, which is a common problem in mesothelioma patients.
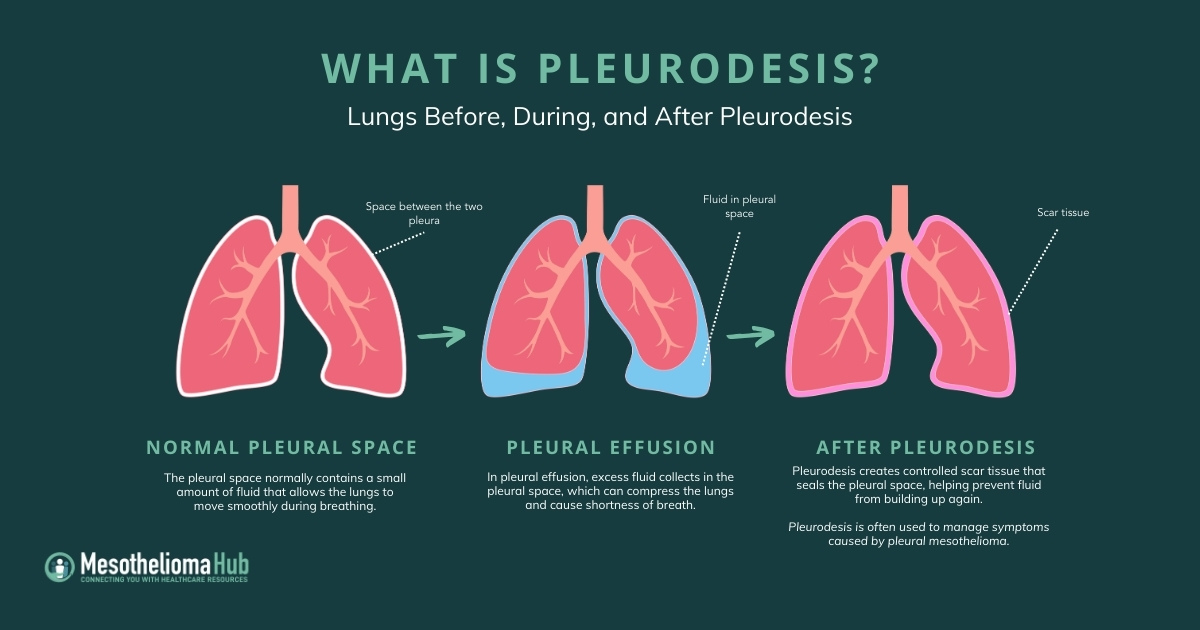
A major symptom of pleural mesothelioma is the buildup of fluid in the pleura, which is located between the layers of tissue that line the lungs and the chest wall. Pleural effusion can lead to coughing, chest pain, and breathing difficulties. If left untreated, it may cause infection or a collapsed lung.
During pleurodesis, specific medicines are injected into the chest cavity between the lungs and chest wall. The medicine creates irritation and swelling between the two layers and adheres them to the chest wall, stopping the buildup of fluid or air.
Pleurodesis may be used as a standalone treatment or combined with another procedure to drain air or fluid around the lungs, called a thoracostomy or thoracoscopy. This procedure is done in the patient’s hospital room. If a thoracostomy or thoracoscopy is combined with pleurodesis, the procedure takes place in an operating room.
Regardless of where the procedure happens, a chest tube will remain in place for up to 48 hours to ensure the lung sticks to the chest wall. Once this is accomplished, it prevents fluid buildup and reduces pain. Patients receive daily X-rays to check their progress.
After the procedure, the chest tube stays in place for 24 to 48 hours, or until the lung has adhered to the chest cavity. Patients who undergo surgery may be required to stay in the hospital so a medical team can track their progress.
Once the chest tube is removed, patients must clean the wound every day. There may be some extra drainage at first, but keeping a bandage over it and changing the dressing regularly will keep the area clean.
Patients should avoid using lotion, taking baths, swimming, or sitting in hot tubs during the recovery process. Patients may also need to take prescriptions to help control pain.
There are other options for mesothelioma patients suffering from pleural effusion or fluid buildup. In a catheter placement procedure, the doctor places a small tube called an indwelling pleural catheter into the patient’s chest. The catheter allows the patient to go home with the small tube and drain the fluids there.
Another alternative to pleurodesis is removing the excess fluid with a needle. This procedure doesn’t require a chest tube. However, this method isn’t permanent, and fluid is likely to return and may require further treatment.
Pleurodesis is an effective procedure. However, there are some risks, which include:
Possible complications of a thoracostomy:
Patients will likely experience some pain or soreness at the site of the chest tube placement. Other possible side effects include fever, shortness of breath, and infection.
Rachel Ernst is a content writer at Mesothelioma Hub. She graduated with a Bachelor of Arts degree from the University of Illinois at Chicago, where she majored in communication and minored in sociology. She hopes to create public awareness about cancer through her writing. In her free time, Rachel likes to be outdoors, watch movies, and spend time with her animals.
Cancer Research UK. (2019). Treatment for Fluid on the Lung (Pleurodesis). Retrieved on October, 18, 2019 from https://mesotheliomahub.com/veterans/veterans-benefits-faq/
Healthline. (n.d.). Pleurodesis. Retrieved on August 2, 2019, from https://healthline.com/health/pleurodesis
Oxford Centre for Respiratory Medicine. (2015). Pleurodesis information for patients. Retrieved on August 2, 2019, from
https://ouh.nhs.uk/patient-guide/leaflets/files/12373Ppleurodesis.pdf
RadiologyInfo. (2018). Chest Tube Placement (Thoracostomy) and Pleurodesis. Retrieved on October, 18, 2019 from https://radiologyinfo.org/en/info.cfm?pg=thoracostomy
UW Health. (2016). What is pleurodesis? Retrieved on August 2, 2019, from https://uwhealth.org/healthfacts/surgery/5847.html